<< Back to Research Summaries
Nationwide ECHO Study Suggests Children in the Western and Southern U.S. May Have Lower Body Mass Index Than Children in the Northeast
Author(s): Dana Dabelea, Jody Ganiban, Traci Bekelman, et al.
Who sponsored this study?
This research was supported by the Environmental influences on Child Health Outcomes (ECHO) program, Office of The Director, National Institutes of Health.
What were the study results?
BMI was lowest for children in the West and South compared to those in the Northeast. When demographic differences were accounted for, children in the Midwest had higher BMIs than those in the Northeast. Across all regions, BMI was highest in children who weighed more at birth and children with less educated mothers. In the Northeast, South, and Midwest, non-Hispanic Black children had higher BMIs on average compared to non-Hispanic white children. In the South and West, BMI was higher for Hispanic white children compared to non-Hispanic white children.
What was the study's impact?
This study revealed some of the regional and demographic factors influencing childhood obesity and overweight. The regional differences in children’s BMI suggest that their surroundings, cultures, and relationships affect the development of childhood obesity. These differences could potentially be linked to variations in food prices, fast food options, and opportunities to exercise.
Why was this study needed?
About 35% of US children are overweight or obese. Childhood obesity can have serious physical and mental health effects that can follow children into adulthood. Understanding the factors that affect children’s weight, can help us create ways to prevent obesity. This study looked at factors related to children’s weight where children live, how much they weighed at birth, and their ethnic background.
Who was involved?
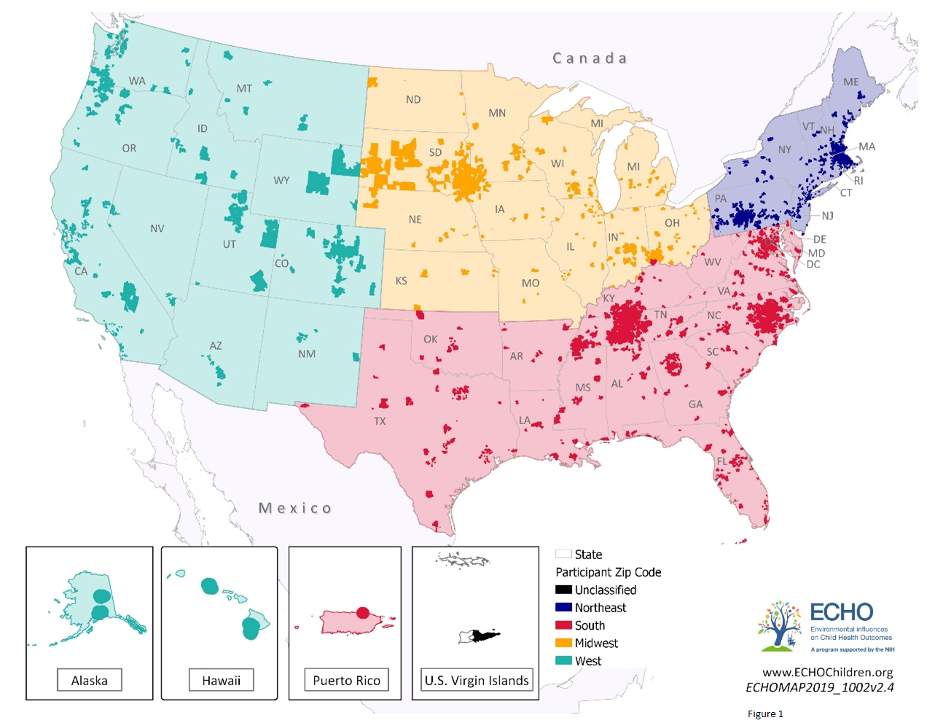
This study included more than 14,000 children and teenagers from birth to age 15. The children lived in the West, South, Northeast, and Midwest regions of the United States. The study included children from different racial and ethnic backgrounds. About half of the children were girls.
What happened during the study?
Doctors measured children’s height and weight from 2000-2018. The research team used this information to calculate each child’s body mass index (BMI), which is an approximate measure of body fat based on height and weight. The team compared differences in average BMI based on region, mother’s level of education, and demographic factors, including birth weight, race, ethnicity, and sex.
What happens next?
More research is needed to understand exactly how regional environments and policies impact children’s BMI and how local policies contribute to differences in obesity risk based on demographics. Identifying the regional and social factors that result in increased obesity risk can help policymakers and public health officials create ways to prevent obesity.
Where can I learn more?
Access the full journal article, titled “Regional and Sociodemographic Differences in Average BMI Among U.S. Children in the ECHO Program” in Obesity.
The content is the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Published: August 31, 2021
Access the associated article.
read more summaries here:
Which Children Develop Asthma in the US
Author(s): Christine Cole Johnson and Aruna Chandran
How Environmental Exposures Affect Child Health Across Multiple Generations
Author(s): Carrie Breton, Rebecca Fry, Alison Hipwell, Cristiane Duarte, Linda Kahn, and Joseph Braun






 the
the 


