About 35% of US children are overweight or obese, increasing their lifetime risk for a variety of negative physical and mental health outcomes. Understanding which environmental, social, and cultural factors contribute to childhood obesity can help doctors and policymakers design strategies for early intervention. ECHO researchers Traci Bekelman, PhD, MPH and Dana Dabelea, MD, PhD of the University of Colorado Anschutz; Jody Ganiban, PhD of George Washington University; and their team explored how regional and demographic factors impact children’s weight. Their research, titled “Regional and Sociodemographic Differences in Average BMI Among U.S. Children in the ECHO Program,” is published in Obesity.
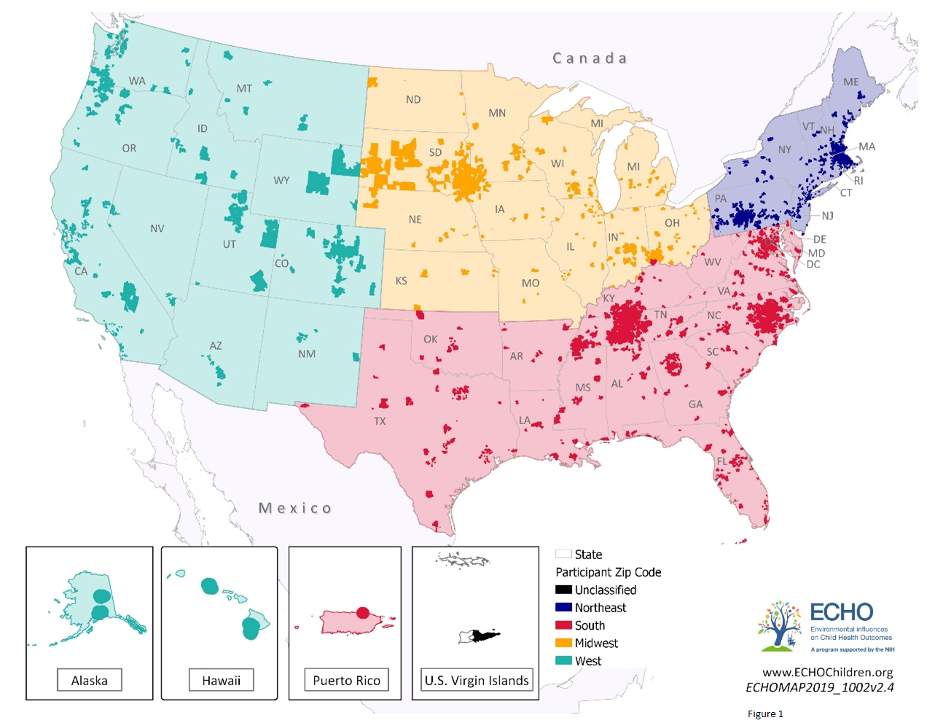
During the study, the team analyzed weight and height data doctors collected between 2000 and 2018 from more than 14,000 children and teens from birth to age 15 located across the US in the West, South, Northeast, and Midwest regions. The data incorporated information from children of various racial and ethnic backgrounds, and approximately half of the children were girls. The team used this data to calculate each child’s body mass index (BMI), an approximate measure of body fat based on height and weight. The team then compared these values based on each child’s birth weight, race, ethnicity, sex, home address, and mother’s level of education.
The study found correlations between the children’s BMI and their location. For example, BMI was lowest in the South and West compared to the Northeast. When demographic differences were accounted for, children in the Midwest had higher BMIs compared to children in the Northeast. More work is needed to understand how regional variations in the price and accessibility of food, the opportunities for physical activity, and the school policies and programs impact childhood obesity risk.
The team also found that children who weighed more at birth and children who had less educated mothers had higher BMIs on average. In the Northeast, South, and Midwest, non-Hispanic Black children had higher BMIs than non-Hispanic white children. And in the South and West, BMI was higher on average for Hispanic white children compared to non-Hispanic white children. This research highlights the need for more thorough investigations into how systemic inequalities contribute to obesity risk in children.
“We were surprised that we only found racial and ethnic differences in BMI in some regions,” said Bekelman. “This finding and future studies could help researchers understand the causes of health disparities.” She also noted that the next step for this research is to investigate which specific regional factors and demographic disparities contribute to higher BMIs.











